We have all heard that breastfeeding is the best way to feed your baby because you can bond with your child and give them the best nutrients and immunity for lifelong health. Besides that, breastfeeding helps moms stay healthy by getting you back to pre-pregnancy weight faster, preventing breast and ovarian cancer, and ensuring heart health. However, sometimes putting baby on the breast is easier said than done – not all moms can breastfeed in the traditional sense of holding your baby to the breast at all times. Moms may not be available if they need to return to work, care for other children, or if their baby stays in the hospital or Neonatal Intensive Care Unit (NICU) after birth.
Enter breast pumps.
Breast pumps have been used for centuries to help moms extract breastmilk to be given later to their baby. There are different pumps to choose from, including manual, battery powered and electric pumps. The best pump for getting milk out are double-electric hospital-grade pumps.

The type of pump you use also matters in terms of potential contamination (i.e., when foreign material can pass into the milk). What matters the most is whether a pump uses an “open” or “closed” system. A “closed” system breast pump has a physical barrier between the parts that touch your breastmilk (flanges, bottles, valves), and the tubing and pump motor (called the “backflow protector”). This keeps your milk sectioned off from the body of the pump. The parts that can easily be cleaned and sterilized are separate from the parts that cannot be cleaned and sterilized, like the interior of the pump motor. This is why hospital grade breast pumps are safe for multiple users – because they have this barrier.
The type of pump you use also matters in terms of potential contamination (i.e., when foreign material can pass into the milk). What matters the most is whether a pump uses an “open” or “closed” system. A “closed” system breast pump has a physical barrier between the parts that touch your breastmilk (flanges, bottles, valves), and the tubing and pump motor (called the “backflow protector”). This keeps your milk sectioned off from the body of the pump. The parts that can easily be cleaned and sterilized are separate from the parts that cannot be cleaned and sterilized, like the interior of the pump motor. This is why hospital grade breast pumps are safe for multiple users – because they have this barrier.
“Open” system breast pumps do not have barriers between the parts that touch your breastmilk and the tubing and pump motor. Because of this, moisture from pumping can enter the tubing and motor. Since mold flourishes in dark, moist places, the open system has a greater risk for mold growth. This means that impossible-to-clean places like the interior of a breast pump motor are very inviting to mold. The most common places to find mold in a breast pump are the tubing, the areas and valves that connect bottles to flanges, and the insides of pumps which have been stored for a long time in a moist basement.
How can I keep mold out of my breast pump and breastmilk?
Prevention of household mold may help prevent mold on your breast pump equipment. Also, a good breast pump should have a protective barrier between the flange (the funnel-shaped part that comes into contact with your breast) and the connected tubing. Pumps without this feature carry extra risk for milk and moisture to get into the tubes and create a breeding ground for mold.

All breast pump parts that come in contact with breastmilk should be cleaned and fully dried after each use. This includes flanges, bottles, valves and breast shields. You can eliminate possible contaminants by washing them with liquid dishwashing soap and warm water. Rinse each piece thoroughly with hot water for 10-15 seconds. Place the pieces neatly on a clean paper towel or on a clean drying rack and allow them to air dry. A dishwasher with a drying cycle can also be used. Avoid using cloth towels to dry your pump parts because they can carry germs and bacteria that are harmful to your breastmilk and your baby.
It is not necessary to clean breast pump tubing unless it comes in contact with breast milk. If you wash your tubing, make sure you hang it to air dry before attaching it to your breast pump. If small water drops (condensation) appear in the tubing after you have pumped, attach the tubes to the pump before you attach your flanges/bottles and turn the pump on for a few minutes until the tubing is dry.
What if I find mold in my breast milk?
At MotherToBaby UR Medicine, we have developed an algorithm (set of rules) to help people manage breastmilk that is potentially contaminated. It is meant to be used in hospitals for sick children, but can be useful for you and your health care provider. Most full-term, healthy, and older infants do not need the precautions outlined below. If you find foreign material in your breastmilk or pump parts, contact your baby’s pediatrician to get advice on what to do.
If your baby is sick or premature, consider sharing the information below with your baby’s provider if you find mold in your breastmilk or pump parts. It is meant to be followed in order from step 1, which includes discarding any milk with foreign material in it (like mold.) Step 2 can help to determine when any other expressed milk may have been affected. For instance, if you know you washed your pump 4 days ago and found the material today, any milk you pumped in the past 4 days could have been contaminated. Contaminated milk could be frozen, which is likely to kill most bacteria and many fungi, or it could be pasteurized using home pasteurization (Step 3). You also need to think about what should be fed to your baby in the meantime: do you have older, stored milk? Do you need donor milk? If you need to use formula, should it be “hypoallergenic?” (Step 4). These are good conversations to have with your baby’s doctor. If you don’t have enough breastmilk, some communities will have breastfeeding medicine specialty providers or lactation consultants who can help mothers with milk supply concerns. You can search for these providers online by clicking here.
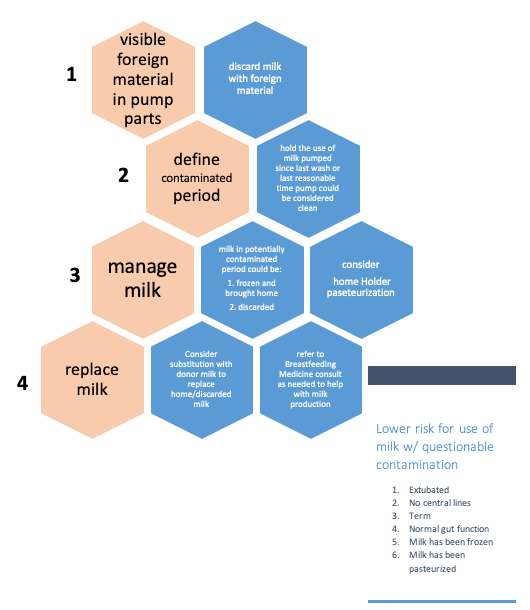
Algorithm for decision-making when pump parts are found to contain foreign material (potential bacteria or fungus). The box at the lower right reminds providers which babies are at lowest risk from drinking milk that has any foreign material in it.
Last, we want to leave you with words of encouragement because we know breastfeeding isn’t easy. It’s downright hard for most. Having that said, please know that resources like MotherToBaby are here for you and just by reading this blog, you’re taking steps to ensure your milk is pumped and stored safely. You’re doing a great job and we can be certain your baby appreciates all you do.
Rogelio Perez D’Gregorio, MD, MS is an Assistant Director of MotherToBaby UR Medicine and Assistant Professor of Obstetrics and Gynecology at the University of Rochester.
Other blog contributions were made by:
Casey Rosen-Carole, MD, MPH, MSEd, FABM, IBCLC is Medical Director of Lactation Services and Programs, Assistant Professor of Pediatrics and OBGYN, and a Consultant for the Lactation Study Center and MotherToBaby URMedicine
Ruth A Lawrence, MD, DD (Hon) FABM, FAAP is Distinguished Alumna Professor Pediatrics and Obstetrics/Gynecology, Northumberland Trust Chair in Pediatrics, UR School of Medicine and Dentistry. Co-Director of the Finger Lakes Children’s Environmental Health Center.
REFERENCES:
Ameda. Is there mold in your breast pump equipment?
Centers or Disease Control and Prevention. Facts about Stachybotrys chartarum and Other Molds.
Eglash A, Liliana Simon L, et al. (2017). ABM Clinical Protocol #8: Human Milk Storage Information for Home Use for Full-Term Infants, Revised 2017. Breastfeed Med.;12(7):390-395.
FDA. U.S. Food and Drugs Administration. Breast pumps.
Hygela Health. Closed System Breast Pumps vs. Open System Breast Pumps.
Jennai L. Moms ABC. How to clean breast pup tubing mold.
La Leche League International. Pumping Milk.
Labiner-Wolfe J, Sara B. Fein SB, Katherine R. Shealy KR, et al. (2008). Prevalence of Breast Milk Expression and Associated Factors. Pediatrics 2008;122:S63–S68.
Magoha H, Kimanya M, De Meulenaer B, et al. (2014). Association between aflatoxin M1 exposure through breast milk and growth impairment in infants from Northern Tanzania. World Mycotoxin Journal. 7(3):277-284.
Spectra. Mould in your Breast Pump Tubing?
Stöppler MC. What is mold?
Walker M. (2012). Pumps and pumping protocols. Clinics in Human Lactation 10. Hale Publishing L.P.